Nicotine and Plastic Surgery: What Patients Need to Know
If you’re considering plastic surgery, one of the most important — and often underestimated — risk factors is nicotine use. Whether it’s cigarettes, vaping, cigars, chewing tobacco, or even nicotine patches and gum, nicotine can significantly impact your surgical outcome. In addition to increasing your risks of surgical complications, you can also experience increased risk of respiratory and cardiac complications from anesthesia.
How Nicotine Affects Healing
Nicotine is a powerful vasoconstrictor, meaning it narrows blood vessels. That restriction reduces blood flow to tissues — and blood flow is essential for:
-
Delivering oxygen
-
Supporting collagen production
-
Preventing infection
-
Promoting proper wound healing
Plastic surgery procedures often involve delicate tissue handling and skin elevation. These tissues rely heavily on strong blood supply to survive and heal properly.When blood flow is compromised, complications increase.
Increased Risks After Plastic Surgery
Patients who use nicotine face significantly higher risks of:
-
Delayed wound healing
-
Wound separation
-
Infection
-
Skin necrosis (tissue death)
-
Poor scarring
-
Implant complications (in breast surgery)
-
Fat necrosis (in procedures involving fat grafting)
In procedures like facelifts, tummy tucks, and breast lifts — where skin is elevated and repositioned — nicotine-related complications can be particularly severe.
Procedures Most Affected by Nicotine
Nicotine is especially dangerous for procedures involving large skin flaps or compromised blood supply, such as:
-
Facelift (Rhytidectomy)
- Nose Job (Rhinoplasty)
-
Tummy Tuck (Abdominoplasty)
- Breast Implants (Breast Augmentation)
-
Breast Lift (Mastopexy)
-
Breast Reduction
-
Body Contouring after Weight Loss
How Long Should You Stop Nicotine Before Surgery?
Most plastic surgeons require patients to stop all nicotine products at least 4–6 weeks before surgery and continue avoiding them for 4–6 weeks after surgery.
Important:
Switching from cigarettes to vaping does not reduce surgical risk if nicotine is still present. Some practices perform nicotine testing before surgery to ensure patient safety.
“But I Only Vape” — Does It Still Matter?
Yes.Even nicotine patches and gum can negatively affect surgical healing because the issue is the nicotine itself — not just smoke.While vaping eliminates some toxins found in cigarette smoke, it does not eliminate the vasoconstrictive effects of nicotine.
What About Marijuana?
Smoking marijuana also affects wound healing due to smoke-related vascular changes and carbon monoxide exposure. If inhaled, it may pose similar surgical risks. This is something patients should discuss openly with their surgeon.
Why Surgeons Are Strict About This Standard
Plastic surgery is often elective. That means your surgeon’s priority is minimizing avoidable risks. Nicotine-related complications can lead to:
-
Additional procedures
-
Permanent scarring
-
Tissue loss
-
Extended recovery time
-
Wound infections
-
Pneumonia
- Death
From a surgeon’s perspective, operating on an active nicotine user significantly increases risk — and many surgeons will postpone surgery until patients are nicotine-free.
The Bottom Line
If you’re investing in plastic surgery, give your body the best possible chance to heal. Quitting nicotine — even temporarily — can dramatically reduce complication rates and improve your aesthetic results.If you’re considering surgery, have an honest conversation with your surgeon about nicotine use. Your safety and outcome depend on it.
Why Submuscular Breast Implants Are Often Better Than Over-the-Muscle Placement
When considering breast augmentation, one of the most important decisions you’ll make with your surgeon is implant placement. Implants can be positioned either over the chest muscle (subglandular), under the chest muscle (submuscular).While both techniques have their place, submuscular placement is often considered the superior option for many patients due to improved aesthetics, safety, and long-term outcomes.

What Is Submuscular Breast Implant Placement?
In submuscular placement, the implant is positioned partially or fully beneath the pectoralis major muscle. This technique provides additional soft tissue coverage over the implant.In contrast, over-the-muscle placement positions the implant directly behind the breast tissue but above the muscle.
1. More Natural-Looking Results
One of the primary advantages of submuscular implants is a more natural contour — especially in patients with thinner breast tissue.Because the muscle provides additional coverage:
-
The upper breast appears softer and more gradual in slope
-
Implant edges are less visible
-
There is reduced risk of visible rippling
For patients with low body fat or minimal existing breast tissue, this added coverage makes a significant difference in achieving a natural aesthetic.
2. Lower Risk of Capsular Contracture
Capsular contracture — a condition where scar tissue tightens around the implant — is one of the most common complications after breast augmentation.
Studies have consistently shown that submuscular placement is associated with a lower rate of capsular contracture compared to over-the-muscle placement. This has been the standard of care for over 50 years. While the exact mechanism isn’t fully understood, improved implant coverage and reduced bacterial contamination risk may play a role.
3. Better Mammogram Visualization
For patients concerned about breast cancer screening, submuscular placement offers an advantage.
Because the implant sits beneath the muscle, there is typically less interference with mammogram imaging. This can improve visualization of breast tissue and may make screening easier for radiologists.
4. Reduced Implant Visibility and Palpability
Submuscular placement reduces:
-
Implant edge visibility
-
Palpable rippling
-
“Implant look” in the upper pole
This is especially important for athletic or thin patients who want discreet, natural-looking enhancement.
5. Improved Long-Term Support
The pectoral muscle provides additional structural support for the implant. Over time, this can help reduce:
-
Bottoming out
-
Excessive downward displacement
-
Premature sagging
While implants are not lifetime devices, submuscular placement often contributes to longer-lasting aesthetic results.
The Bottom Line
For many patients, submuscular breast implant placement provides:
-
More natural aesthetics
-
Lower complication rates
-
Better long-term outcomes
-
Improved imaging compatibility
That said, breast augmentation is not one-size-fits-all. The best results come from individualized planning, surgical expertise, and clear communication about your aesthetic goals.
Dr. Graham is an expert in Breast Surgery in Rochester, NY. If you’re considering breast augmentation, schedule a consultation to discuss which implant placement is right for you — and how we can create results that look beautifully natural and uniquely yours.
Ozempic Body: Understanding the Physical Changes That Can Follow Weight Loss Medications
GLP-1 medications like Ozempic®, Wegovy®, and Mounjaro® have transformed the weight-loss conversation. While many patients celebrate meaningful and life-changing weight reduction, a new term has entered popular culture: “Ozempic Body.”This phrase refers to the physical changes some individuals notice after rapid or significant weight loss—particularly changes in skin tone, volume, and body contours.Understanding what “Ozempic Body” means, why it happens, and what options exist can help patients feel informed and empowered as they navigate their aesthetic goals.
What Is “Ozempic Body”?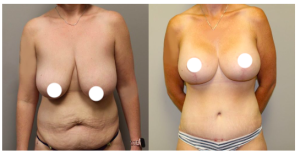
“Ozempic Body” is not a medical diagnosis. It’s a colloquial term used to describe body contour changes that can occur after substantial weight loss, especially when weight is lost quickly.Common concerns associated with Ozempic Body include:
-
Loose or sagging skin in the abdomen, arms, thighs, or buttocks
-
Loss of volume in the breasts or buttocks
-
A “deflated” or less firm appearance in certain areas
-
Changes in skin elasticity and texture
These changes are not unique to Ozempic—they can happen with any significant weight loss, whether achieved through medication, bariatric surgery, or lifestyle changes.
Why Does Ozempic Body Happen?
1. Rapid Weight Loss
When weight is lost quickly, the skin may not have enough time to retract and tighten, especially in areas that have been stretched for years.
2. Loss of Fat Volume
Fat provides structure and fullness. When fat volume decreases, it can reveal lax skin or lead to contour irregularities.
3. Age and Skin Elasticity
As we age, collagen and elastin levels decline, making it harder for skin to bounce back after weight loss.
4. Genetics
Some people are genetically predisposed to better skin retraction than others.
Is Ozempic Body Preventable?
Not entirely—but certain factors may help minimize its appearance:
-
Gradual, supervised weight loss when possible
-
Strength training to preserve muscle tone
-
Adequate protein intake and hydration
-
Good skincare habits and sun protection
Even with these measures, some degree of skin laxity or volume loss is normal after significant weight reduction.
Aesthetic Options for Addressing Ozempic Body
For patients who are happy with their weight loss but unhappy with body contours, aesthetic medicine and plastic surgery can offer solutions tailored to individual needs.
Non-Surgical Options May Include:
-
Skin-tightening technologies (radiofrequency or ultrasound-based treatments)
-
Injectable fillers or biostimulants to restore volume in select areas
-
Non-surgical body contouring treatments
Surgical Options May Include:
-
Tummy tuck (abdominoplasty)
-
Arm lift (brachioplasty)
-
Thigh lift
-
Breast lift with or without augmentation
-
Body lift procedures for more extensive skin laxity
A consultation with a board-certified plastic surgeon is the best way to determine which options are appropriate.
Weight Loss Is a Success—Refinement Is a Personal Choice
It’s important to emphasize that Ozempic Body does not mean weight loss failed. On the contrary, it often reflects a major health achievement. Weight loss is associated with innumerable health benefits including improving cardiovascular, musculoskeletal, and even mentall health. Furthermore, it decreases cancer risk and overall body inflammation. Choosing to address body contour concerns afterward is not about vanity—it’s about optimizing health while aligning the outside with how patients feel on the inside.
Final Thoughts
GLP-1 medications have opened new doors for weight management, but they can also introduce unexpected aesthetic changes. Understanding Ozempic Body helps normalize the conversation and reminds patients that options exist. In addition, the bariatric surgery literature shows that patients who undergo cosmetic skin removal after weight loss are much less likely to undergo weight regain, a common problem with GLP-1 medications after their cessation.
If you’ve experienced physical changes after weight loss and want to explore ways to restore balance, confidence, and contour, a personalized consultation can help map out the next steps. Dr. Graham is an expert in breast and body surgery, learning his craft at a major bariatric center in Ohio. He has over 20 years of experience and innate artistic ability.
Ozempic Breasts: What It Is, Why It Happens, and What You Can Do
As medications like Ozempic® (semaglutide) continue to grow in popularity for weight loss and diabetes management, new terms are emerging online—one of the most talked about being “Ozempic breasts.”
If you’ve noticed changes in breast size, shape, or firmness while losing weight on Ozempic, you’re not alone. The good news? These changes are common, expected, and manageable.
Let’s break down what “Ozempic breasts” really means, why it happens, and what options exist to address it.
What Are “Ozempic Breasts”?
“Ozempic breasts” is a non-medical term used to describe changes in breast appearance after significant weight losswhile taking GLP-1 medications like Ozempic.
Common changes include:
- Loss of breast volume
- Increased sagging or ptosis
- Softer or deflated appearance
- Changes in breast symmetry
Importantly, Ozempic itself does not directly affect breast tissue. These changes are the result of fat loss, not the medication targeting the breasts.
Why Does Ozempic Cause Breast Changes?
- Breasts Are Largely Made of Fat
Breasts are composed of:
- Fat
- Glandular tissue
- Connective tissue and skin
When weight loss occurs—especially rapid or significant weight loss—the fat volume in the breasts often decreases.
- Rapid Weight Loss Affects Skin Elasticity
GLP-1 medications can lead to faster weight loss than traditional methods. When this happens:
- Skin may not have time to retract
- Breast tissue can lose structural support
- Sagging becomes more noticeable
Age, genetics, and prior pregnancies can increase this effect.
- Hormonal Changes and Aging Play a Role
As we age, natural decreases in estrogen reduce skin elasticity and collagen production, making breast changes more noticeable during weight loss.
Is This Unique to Ozempic?
No. Similar changes have been observed with:
- Bariatric surgery
- Diet-induced weight loss
- Pregnancy and postpartum weight loss
“Ozempic breasts” is simply a modern label for a long-recognized consequence of weight loss.
Can You Prevent Ozempic Breasts?
While you can’t completely prevent breast changes during weight loss, you can minimize their severity:
✔ Gradual Weight Loss (When Possible)
Slower weight loss allows skin more time to adapt.
✔ Proper Nutrition
Adequate protein supports skin integrity and collagen production.
✔ Supportive Bras
Well-fitted bras reduce strain on breast skin during weight changes.
Surgical Options After Weight Loss
🔹 Breast Augmentation
Restores lost volume using implants. The only way to get perkiness is with a breast implant.
🔹 Breast Lift (Mastopexy)
Addresses sagging and repositions the nipple.
🔹 Augmentation + Lift
Combines volume restoration with reshaping for comprehensive results. This can be done as a single or two stage operation depending on your anatomy and surgeon’s experience.
Many surgeons recommend waiting until weight stabilizes before considering surgery. A stable weight for at least 3-6 months is recommended. Reaching you ideal weight is essential for long lasting results.
When Should You See a Specialist?
Consider consulting a board-certified plastic surgeon if:
- Breast changes are affecting your confidence
- Weight has been stable for several months
- Non-surgical options are insufficient
A personalized consultation can determine the best approach for your goals. Dr. Graham is an expert in cosmetic breast surgery, having over 20 years of experience.
Can You Use an HSA for Plastic Surgery Procedures?
Patients often ask whether Health Savings Accounts (HSAs) can be used to pay for plastic surgery. The answer depends on one key factor: medical necessity. While most cosmetic procedures are not HSA-eligible, certain plastic and reconstructive surgeries may qualify when they are performed to treat a medical condition—not just to improve appearance. Below, we explain what patients should know before using HSA funds.
Understanding the IRS Rules
The IRS allows HSA funds to be used for medical care that is intended to:
- Diagnose
- Treat
- Mitigate
- Prevent a disease or medical condition
Procedures performed solely for cosmetic reasons are generally not eligible for HSA reimbursement.
Procedures That Are Not HSA-Eligible
Purely elective cosmetic procedures typically do not qualify, including:
- Cosmetic breast augmentation
- Facelifts
- Liposuction for aesthetic purposes
- Botox or fillers for wrinkles
- Non-medical body contouring
These treatments are considered appearance-enhancing rather than medically necessary.
When Plastic Surgery May Be HSA-Eligible
Certain plastic surgery procedures may qualify for HSA use when they address a documented medical concern.
Examples include:
- Breast reduction to relieve chronic neck, back, or shoulder pain
- Rhinoplasty to correct breathing problems (such as a deviated septum)
- Upper Eyelid Surgery(Upper Blepharoplasty) when extra skin obstructs your vision
- Reconstructive surgery following cancer, trauma, or congenital conditions
- Excess skin removal(abdominoplasty) after significant weight loss when it causes rashes, infections, or functional limitations
- Umbilical Hernia Repair repaired at the time of abdominoplasty
- Botox for medical indications such as migraines, TMJ disorders, or excessive sweating
In these cases, the goal of surgery is health improvement—not cosmetic enhancement.
The Importance of Medical Documentation
For HSA eligibility, patients typically need a Letter of Medical Necessity (LMN) from a qualified healthcare provider. This letter should explain:
- The medical condition being treated
- Why the procedure is necessary
- How surgery will improve or alleviate symptoms
Without proper documentation, HSA claims may be denied if audited.
Procedures with Both Medical and Cosmetic Components
Some surgeries include both functional and aesthetic elements. In these situations:
- The medically necessary portion may be HSA-eligible
- The cosmetic portion is not
For example:
- Septoplasty (functional) + cosmetic rhinoplasty
- Septoplasty → HSA eligible
- Cosmetic rhinoplasty → Not eligible
Itemized billing is essential in these cases.
Are Consultations Covered by an HSA?
- ✔ Consultations related to evaluating a medical condition may qualify
- ❌ Cosmetic-only consultations generally do not
Patients should confirm eligibility before using HSA funds.
What Happens If HSA Funds Are Used Incorrectly?
Using HSA money for non-eligible cosmetic procedures may result in:
- The amount being treated as taxable income
- A potential 20% IRS penalty (unless the account holder is over age 65)
This is why verification and documentation are so important.
Our Recommendation to Patients
Before planning to use HSA funds for any plastic surgery procedure, we recommend that patients:
- Discuss medical symptoms with their provider
- Obtain a Letter of Medical Necessity, if applicable
Final Thoughts
While most cosmetic procedures are not HSA-eligible, many reconstructive and medically necessary plastic surgery procedures may qualify. Discuss the possibility of using your HSA or FSA with your plastic surgeon. They may be willing to work with you for full or partial payment. Dr. Graham and his staff will do all they can to facilitate using HSA/FSA funds to help finance your surgery.
ENT vs. Plastic Surgeon for Cosmetic Rhinoplasty
Patients considering rhinoplasty often ask whether an ENT (ear, nose, and throat) surgeon or a plastic surgeon is the better choice for cosmetic nose surgery. The answer isn’t about which specialty is “better”—it’s about choosing a surgeon with the right training, experience, and focus on rhinoplasty.
Both ENT surgeons and plastic surgeons can achieve excellent cosmetic results when rhinoplasty is a core part of their practice.
Understanding the Difference in Training
ENT Surgeons
ENTs (otolaryngologists) are specialists in the anatomy and function of the nose and airway. Their training emphasizes:
- Nasal airflow and breathing
- Septal deviation and structural support
- Nasal trauma and reconstruction
- Functional nasal surgery
Plastic Surgeons
Plastic surgeons are trained in aesthetic surgery of the nose, face and body, with emphasis on:
- Facial balance and proportion
- Soft tissue sculpting
- Scar placement and healing
- Cosmetic harmony
Plastic surgeons often bring a refined artistic perspective to cosmetic nasal reshaping.
Who Performs Better Cosmetic Rhinoplasty?
There is no single specialty that consistently produces better cosmetic rhinoplasty results. Outcomes depend on:
- The surgeon’s rhinoplasty experience and volume
- Specialized training in facial plastic surgery
- Mastery of both nasal function and aesthetics
- Experience with complex and revision cases
- Consistently strong before-and-after results
A surgeon who performs rhinoplasty frequently—rather than occasionally—will typically achieve more predictable, refined outcomes.
When an ENT May Be the Right Choice-Functional Issues
An ENT surgeon may be particularly well suited if your rhinoplasty involves both functional and cosmetic concerns, such as:
- Chronic nasal obstruction or breathing difficulty
- Deviated septum
- Turbinate enlargement
- Nasal trauma or prior injury
- The need for septoplasty alongside cosmetic refinement
ENTs with advanced facial plastic training are uniquely equipped to preserve or improve breathing while reshaping the nose.
When a Plastic Surgeon May Be the Right Choice-Cosmetic Appearance
A plastic surgeon may be ideal if your goals are primarily cosmetic, including:
- Refining the nasal tip
- Improving nasal symmetry
- Reducing nasal width or profile irregularities
- Enhancing overall facial harmony
Plastic surgeons often excel in achieving subtle aesthetic refinements that complement the rest of the face.
What Matters Most When Choosing a Rhinoplasty Surgeon
Rather than focusing solely on a surgeon’s specialty, patients should consider:
- Board certification and advanced training
- A strong focus on rhinoplasty within the practice
- A robust gallery of rhinoplasty-specific results
- Experience with revision rhinoplasty
- Clear communication and personalized treatment planning
Final Thoughts
Both ENT surgeons and plastic surgeons can perform exceptional cosmetic rhinoplasty. The most important factor is selecting a surgeon who specializes in rhinoplasty, understands nasal function, and consistently delivers results that align with your aesthetic goals.
Dr. Graham is an expert in both primary and revision rhinoplasty. He has trained with the masters from across the globe to perfect his craft. He offers the latest technology, including waterjet rhinoplasty.
